Why Medicare Enrollment Timing Matters More Than You Think
Medicare enrollment and deadlines determine when you can get coverage, what it will cost, and whether you’ll face lifelong penalties. Here’s what you need to know:
Key Medicare Enrollment Periods:
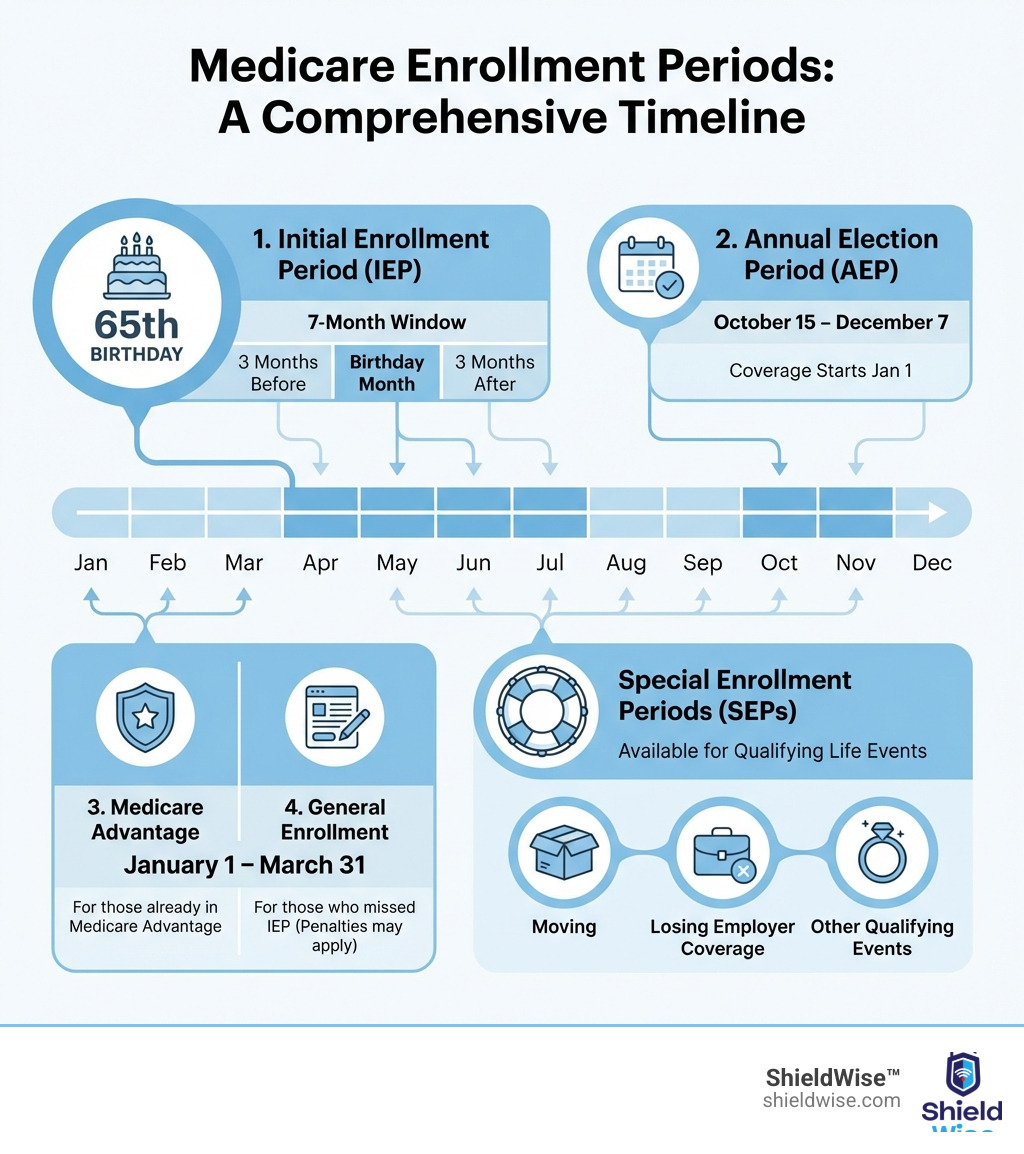
- Initial Enrollment Period (IEP) – A 7-month window around your 65th birthday.
- Annual Election Period (AEP) – October 15 to December 7 each year to change plans.
- Medicare Advantage Open Enrollment Period (MAOEP) – January 1 to March 31 for those in a Medicare Advantage plan.
- General Enrollment Period (GEP) – January 1 to March 31 for those who missed their IEP; penalties may apply.
- Special Enrollment Periods (SEPs) – For qualifying life events like losing employer coverage.
Missing your deadline can mean:
- Waiting months to enroll
- Paying a permanent late enrollment penalty (10% more for each 12-month period you delay Part B)
- Coverage gaps that leave you uninsured
With 22% of enrollees finding the sign-up process difficult, understanding when you can enroll is critical. Knowing these deadlines can save you thousands of dollars and prevent months of confusion.
At ShieldWise, we help you steer Medicare enrollment and deadlines without the sales pressure or jargon. Our goal is to give you the facts and confidence to make the right decision for your situation.
The Initial Enrollment Period (IEP): Your First Window to Enroll

The Initial Enrollment Period (IEP) is your first chance to sign up for Medicare. This 7-month window is centered around your 65th birthday:
- The three months before the month you turn 65
- The month you turn 65
- The three months after the month you turn 65
For example, a May birthday means your IEP runs from February 1st to August 31st. If your birthday is on the first of the month, your IEP starts and ends one month earlier.
You’ll be automatically enrolled in Medicare Part A and B if you’re already receiving Social Security or Railroad Retirement Board (RRB) benefits for at least four months before turning 65. If so, your card will arrive about three months before your birthday. Otherwise, you must sign up yourself. Even with automatic enrollment, you can delay Part B if you have other creditable coverage, like from an employer.
Coverage starts on the first of the month. If you enroll in the three months before your birthday, coverage begins in your birthday month. If you enroll during or after your birthday month, your coverage will be delayed by one to three months. For a more detailed look at this milestone, check out our guide for those turning 65.
How to enroll if you’re not automatically signed up
If you need to sign up for Medicare manually, the Social Security Administration (SSA) offers three ways to apply:
- Online: The fastest method is through the Social Security website. You’ll need a “my Social Security” account, and the application can take as little as 10 minutes.
- By Phone: Call Social Security at 1-800-772-1213 (TTY: 1-800-325-0778).
- In-Person: Visit a local Social Security office. It’s best to make an appointment to avoid long waits.
For comprehensive instructions, refer to our guide on how to sign up for Medicare.
What’s the difference between the IEP and Open Enrollment?
It’s easy to confuse the Initial Enrollment Period (IEP) with the Annual Election Period (AEP), often called “Open Enrollment.” Here’s the difference:
The Initial Enrollment Period (IEP) is your one-time window to sign up for Medicare for the first time, usually when you turn 65. This is when you enroll in Part A and Part B and can also choose a Medicare Advantage (Part C) or Prescription Drug (Part D) plan.
The Annual Election Period (AEP), or Open Enrollment, is an annual period from October 15th to December 7th for people already on Medicare. It’s your yearly chance to review and change your existing health or drug plans for the next year, not for first-time enrollment in Original Medicare.
Think of the IEP as your initial sign-up and AEP as your annual plan review. For a deeper dive, explore our understanding Medicare coverage options guide.
Key Medicare Enrollment and Deadlines: Other Important Timelines
Once you’re enrolled in Medicare, it’s important to review your coverage annually, as plans can change their costs, coverage, and provider networks. Understanding the following enrollment periods is key to ensuring your plan continues to meet your needs.
The Annual Election Period (AEP) / Open Enrollment
The Annual Election Period (AEP), or Medicare Open Enrollment, runs from October 15 to December 7 each year. This is your annual opportunity to make changes to your Medicare health and drug coverage for the following year, with any changes taking effect on January 1st.
During AEP, you can:
- Switch from Original Medicare to a Medicare Advantage Plan (Part C), or vice versa.
- Switch from one Medicare Advantage Plan to another.
- Join, drop, or switch a Medicare Prescription Drug Plan (Part D).
This period is vital for reviewing your plan’s “Annual Notice of Change” (ANOC) to see what’s new. If you’re satisfied with your current plan and it’s still offered, you don’t need to do anything; your coverage will generally renew automatically. Our compare Medicare Advantage plans guide can help you evaluate your options. For official guidance, you can also learn more about Medicare Open Enrollment from Medicare.gov.
The Medicare Advantage Open Enrollment Period (MAOEP)
The Medicare Advantage Open Enrollment Period (MAOEP) runs from January 1 through March 31 each year. This period is specifically for individuals already enrolled in a Medicare Advantage Plan, giving you a second chance to make a change.
During the MAOEP, you can make one of the following changes:
- Switch to another Medicare Advantage Plan.
- Drop your Medicare Advantage Plan and return to Original Medicare (you can also join a Part D plan at this time).
Your new plan choice will take effect the first of the month after your request. This period is not for switching from Original Medicare to Medicare Advantage. For a deeper dive, explore our complete guide to Medicare Advantage.
The General Enrollment Period (GEP)
If you missed your Initial Enrollment Period (IEP) and don’t qualify for a Special Enrollment Period, you can enroll during the General Enrollment Period (GEP) from January 1 through March 31 each year.
The GEP is for those who need to sign up for Medicare Part B (or premium Part A) after their initial eligibility has passed. Your coverage will take effect the first of the month after you enroll. However, enrolling during the GEP often results in a lifelong late enrollment penalty if you didn’t have other creditable coverage. You can read the CMS fact sheet on enrollment changes for more details.
Navigating Special Enrollment Periods (SEPs)

Life changes can trigger a Special Enrollment Period (SEP), allowing you to enroll in or change your Medicare coverage outside of the standard windows, often without penalty. SEPs are designed to prevent gaps in health coverage after specific “qualifying life events.”
How employer coverage impacts your medicare – enrollment and deadlines
One of the most common SEPs relates to employer health coverage. If you continue working past age 65 and have “creditable” health insurance from your or your spouse’s employer, you can typically delay Medicare Part B without penalty.
When you lose or leave that job or coverage, you’ll usually qualify for an 8-month SEP to sign up for Part B without penalty. This window starts the month after your employment or group health plan coverage ends, whichever is first.
It’s important to know that COBRA, retiree health plans, and VA coverage generally do not count as creditable coverage that allows you to delay Part B enrollment without penalty. The rules can be complex, so it’s always best to verify your situation. For more information, you can learn about SEPs for unique situations at Medicare.gov.
Other common reasons for a Special Enrollment Period
Beyond employer coverage, various other life events can trigger an SEP, allowing you to adjust your Medicare enrollment and deadlines.
Here are some common qualifying events:
- Moving: If you move out of your plan’s service area or to an area with new plan options.
- Qualifying for Extra Help: If you become eligible for Medicare’s program to help with prescription drug costs. To see if you qualify, find out if you qualify for Extra Help.
- Losing other coverage: This includes losing Medicaid or your plan leaving the Medicare program.
- Exceptional Circumstances: Situations beyond your control, like a natural disaster or receiving inaccurate information from a plan.
- Release from Incarceration.
- The 5-Star Enrollment Period: This unique SEP runs from December 8 through November 30 and allows you to switch once to a Medicare plan with a 5-star quality rating.
The duration and rules for an SEP vary by event, so it’s crucial to confirm your eligibility and timeline with Medicare or Social Security.
The High Cost of Waiting: Penalties and Coverage Gaps
Overlooking Medicare enrollment and deadlines can lead to significant financial penalties and dangerous gaps in your health coverage. These consequences can last a lifetime and often begin when someone misses their Initial Enrollment Period (IEP) without having other qualifying coverage.
What are the consequences of missing medicare – enrollment and deadlines?
Failing to enroll on time can be costly:
- Part B Late Enrollment Penalty: If you delay Part B enrollment without having other creditable coverage, you may face a penalty. This is an extra 10% of the standard premium for each full 12-month period you were eligible but didn’t sign up. This penalty is added to your monthly premium for as long as you have Part B.
- Part A Premium Penalty: Most people get premium-free Part A. However, if you have to buy it and you delay, your monthly premium may increase by 10%. You’ll pay this higher premium for twice the number of years you delayed enrollment.
- Part D Late Enrollment Penalty: If you go without Part D or other creditable drug coverage for 63 consecutive days or more after your IEP ends, you’ll likely pay a penalty. It’s calculated by multiplying 1% of the “national base beneficiary premium” by the number of uncovered months and is added to your monthly Part D premium for life.
Beyond penalties, delaying enrollment can leave you uninsured, exposing you to high medical bills. Our guide to Medicare out-of-pocket costs can provide valuable insights. To learn how to avoid these extra charges, Medicare.gov offers guidance on how to avoid late enrollment penalties.
Your Step-by-Step Guide to Applying for Medicare
Applying for Medicare for the first time can seem daunting, but breaking it down into manageable steps makes the journey smoother. Here’s what you need to know about the application process, required documents, and when your coverage will begin.
What documentation is needed to apply for Medicare?
To ensure a smooth application process, it’s helpful to have certain documents and information ready:
- Social Security Number
- Birth Certificate (or city/state of birth)
- Proof of U.S. Citizenship or Legal Residency (e.g., passport or Permanent Resident Card)
- Employment Information for you and your spouse
- Current Health Insurance Information, including start and end dates for any group health plans.
Having this information organized will speed up your application. The Social Security Administration provides a helpful checklist for online Medicare, retirement, and spouses applications.
Can I enroll in Medicare if I have a Health Savings Account (HSA)?
Yes, but the rules are tricky and can lead to tax penalties if not handled correctly. You cannot contribute to an HSA once you are enrolled in any part of Medicare, including premium-free Part A.
Because Medicare Part A coverage can be retroactive up to six months from when you apply, any HSA contributions made during that retroactive period may be subject to taxes and penalties. To avoid this, it’s recommended to stop contributing to your HSA at least six months before you plan to enroll in Medicare.
For detailed information on how HSAs interact with Medicare, consult official resources like the IRS. You can learn more about HSAs and Medicare at IRS.gov.
When does my Medicare coverage start after enrolling?
Your Medicare coverage always starts on the first day of the month, but the exact date depends on when you enroll.
- Initial Enrollment Period (IEP): If you enroll in the 3 months before your 65th birthday, coverage starts the month you turn 65. If you enroll during your birthday month or later, your start date will be delayed.
- General Enrollment Period (GEP): When you enroll between January 1 and March 31, your coverage starts on the first day of the month after you enroll.
- Special Enrollment Periods (SEPs): Coverage start dates vary, but it’s often the first of the month after your plan receives your enrollment request.
For specifics, visit Medicare.gov’s page on when does Medicare coverage start?.
Conclusion
Navigating Medicare enrollment and deadlines is critical to securing your health coverage and avoiding unnecessary penalties. We’ve explored your Initial Enrollment Period, the Annual Election Period for changing plans, and other key timelines like the MAOEP, GEP, and flexible Special Enrollment Periods.
Missing these deadlines can lead to lifelong penalties and dangerous gaps in your coverage. At ShieldWise, we believe understanding your options should be empowering, not overwhelming. We’re here to provide clear, jargon-free guidance to help you make these important decisions without confusion or costly mistakes. Proactive engagement with your Medicare enrollment and deadlines ensures you’re protected.
Ready to take control of your Medicare journey? Let us help you compare plans and make informed choices. Secure your future with the right coverage for seniors.
